What is cartilage, and what does it do?
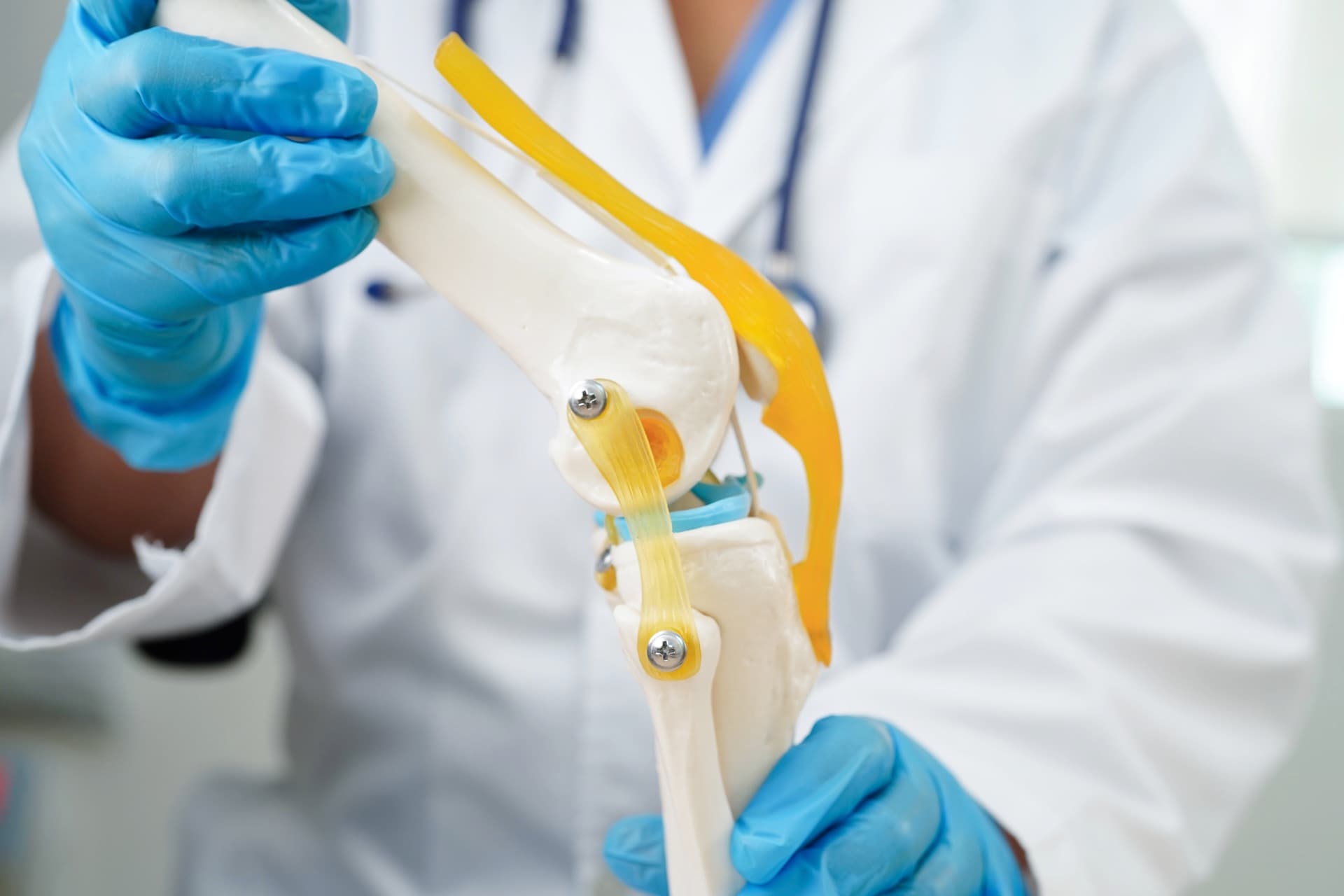
Cartilage is the smooth, specialised lining on the surface of a joint. Its job is to absorb load, reduce shock, and allow the joint surfaces to glide smoothly against each other.
It is one of the key tissues that keeps a joint functioning well. When cartilage becomes damaged, the joint loses that smooth protective surface. Over time, that can lead to pain, swelling, stiffness, inflammation, and eventually arthritis.
Cartilage is not just a passive lining. It is central to how the joint moves, copes with force, and stays healthy over time.